Blog
Recent Posts
- Cosmetic Dentistry in Onalaska: Brighten and Enhance Your Smile at Onalaska Smiles Dental
February 12, 2026Cosmetic Dentistry in Onalaska; Your smile is one of the first things people notice about you. A bright, balanced smile can boost confidence, improve how you feel in social and professional situations, and enhance your overall appearance. If you’ve ever felt self-conscious about the color or shape of your teeth, cosmetic dentistry provides effective solutions to help you achieve a smile you love.
At Onalaska Smiles Dental in Onalaska, cosmetic dentistry focuses on two highly effective treatments: teeth whitening and dental veneers. These services are designed to address common cosmetic concerns, from stubborn discoloration to uneven or imperfect tooth surfaces, giving you a revitalized smile that looks natural and feels great.
What Is Cosmetic Dentistry?
Cosmetic dentistry is a branch of dental care that focuses on improving the visual appearance of your teeth and smile. While general dentistry ensures that your teeth and gums are healthy and functioning properly, cosmetic dentistry enhances how your teeth look — including color, shape, symmetry and overall harmony.
Whether you’re seeking a subtle refresh or a more significant transformation, cosmetic treatments can be personalized to match your goals and lifestyle.
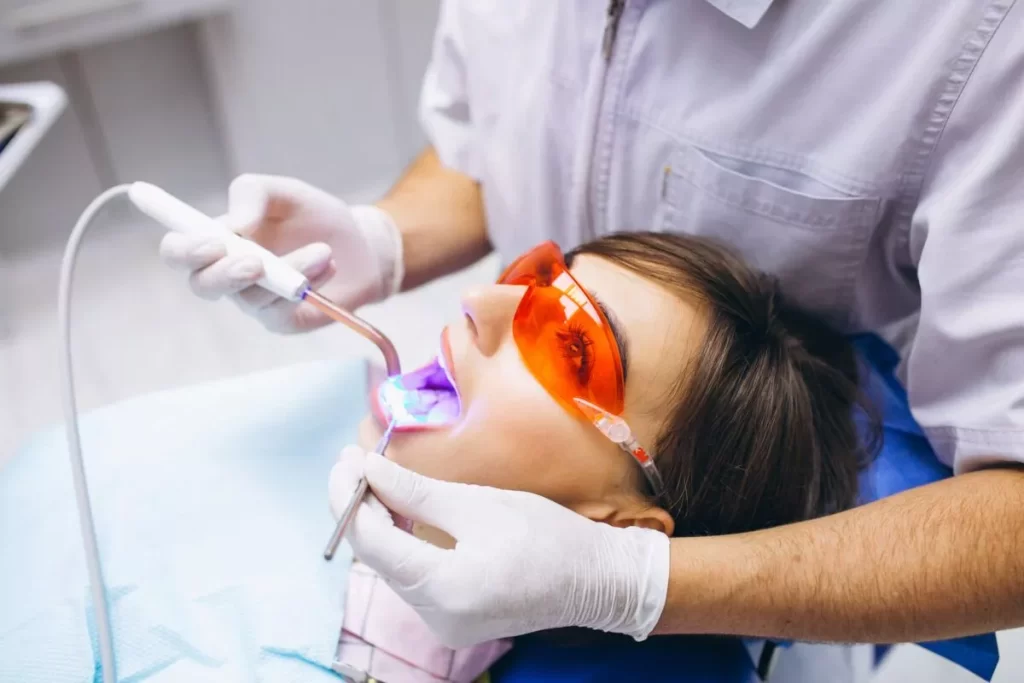
Professional Teeth Whitening: Brighten Your Smile
One of the most sought-after cosmetic treatments available at Onalaska Smiles Dental is professional teeth whitening. Teeth can become stained or discolored over time due to many everyday activities — including drinking coffee, tea or soda, consuming dark-colored foods, smoking and even the natural aging process. While over-the-counter products may offer minimal results, professional whitening delivers stronger, more consistent improvements.
How Teeth Whitening Works
Professional teeth whitening uses a custom-formulated whitening gel that is applied directly to the surface of your teeth. This gel works by breaking down stubborn stains that have formed over time, helping to expose a brighter, cleaner shade underneath. The process is tailored to your specific needs, ensuring safety and effectiveness.
In many cases, patients notice a visible difference in the brightness of their smile after just one whitening session. These treatments can be done in-office for rapid results, or sometimes offered with take-home professional whitening systems that allow you to whiten gradually from your own home under guidance.
Benefits of Professional Whitening
- More dramatic results than store-bought products — Professional whitening targets deep stains that over-the-counter products often cannot reach.
- Customized treatment — Your dental team evaluates your individual needs and provides the best approach for your smile.
- Boost in self-confidence — A brighter smile often makes patients feel more comfortable and confident in all areas of life.
After professional whitening, maintaining good oral hygiene and reducing habits that stain enamel will help prolong your results
Dental Veneers: Transform Imperfections Into Confidence
While teeth whitening improves color, dental veneers offer a powerful cosmetic solution that covers multiple concerns at once. Veneers are highly effective for patients who want a more dramatic improvement in both the look and symmetry of their teeth.
What Are Dental Veneers?
Dental veneers are ultra-thin, custom-crafted shells that fit over the front surfaces of your teeth. They are typically made from high-quality materials that mimic the appearance of natural enamel. When bonded to your teeth, veneers conceal imperfections and create a more uniform, polished smile.
Veneers can address a variety of cosmetic concerns, such as:
- Deep or stubborn discoloration that doesn’t respond well to whitening.
- Chipped or worn enamel.
- Irregular tooth shape or size.
- Uneven spacing or gaps between teeth.
- Surface imperfections or minor alignment issues.
Because veneers cover the visible front portion of your teeth, they provide comprehensive aesthetic improvements in color, shape and symmetry — creating a smile that looks balanced and vibrant.
The Veneers Process
The process of getting veneers typically begins with a consultation at Onalaska Smiles Dental to discuss your goals and evaluate your dental health. During this appointment, your dental team will explain what to expect and help you decide if veneers are the right option.
Once a plan is agreed upon, a small amount of enamel may be gently prepared so the veneers fit comfortably and naturally. Impressions are taken and custom veneers are fabricated to match the shape and shade that best complements your smile. After fabrication, the veneers are securely bonded to the teeth, instantly enhancing overall appearance.
Benefits of Dental Veneers
- Natural, long-lasting results — Veneers are designed to resemble real enamel and remain durable over time.
- Comprehensive cosmetic improvement — They address multiple issues in one treatment, including shape and color imperfections.
- Boost in appearance and confidence — A more symmetrical, balanced smile often makes patients feel more self-assured.
Dental veneers are perfect for patients who want more than just whiter teeth — especially when combined concerns like shape and color influence the overall look of their smile.
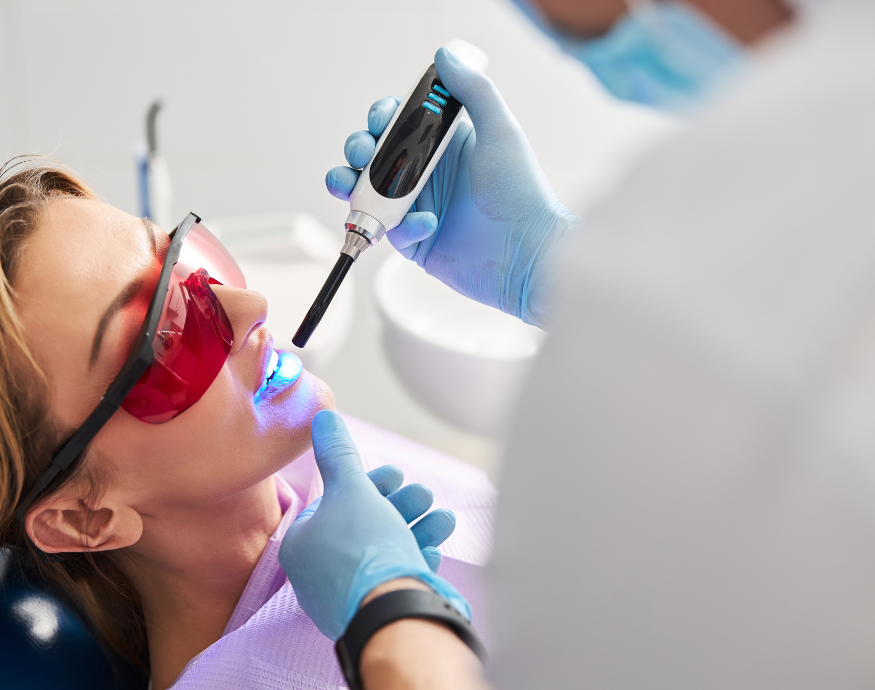
Why Cosmetic Dentistry Matters
Enhancing your smile through cosmetic dentistry can have a positive impact on your life in many ways:
- Improved self-confidence — Many patients report feeling more confident in everyday interactions after cosmetic treatment.
- Enhanced appearance — Whiter, well-shaped teeth can balance facial features and elevate your overall look.
- Better long-term satisfaction — Investing in how your smile looks can improve how you feel about yourself today and in the future.
Cosmetic dentistry doesn’t just change how your teeth look — it often changes how you feel, how you interact with others and how you present yourself.
Caring for Your Cosmetic Results
After receiving cosmetic treatment, maintaining good oral hygiene helps preserve your results. Recommended practices include:
- Brushing and flossing daily to protect both natural teeth and any cosmetic enhancements.
- Regular dental checkups to ensure ongoing oral health and monitor condition of veneers.
- Limiting foods and drinks that stain enamel to help your whitening results last longer.
Good at-home care supports the longevity of your cosmetic improvements and keeps your smile healthy overall.
Cosmetic dentistry at Onalaska Smiles Dental in Onalaska offers effective ways to enhance your smile through professional teeth whitening and custom dental veneers. Whether you want a brighter smile or a complete cosmetic transformation, these treatments can help you achieve the smile you’ve always wanted.
Contact us today to schedule your appointment.
- Restorative Dentistry in Onalaska
January 28, 2026Restorative Dentistry in Onalaska; A confident, healthy smile doesn’t just look good — it supports how you eat, speak and feel every day. But when dental issues such as decay, damage or missing teeth impact the way your mouth works, restorative dentistry can help restore both function and appearance. At Onalaska Smiles Dental in Onalaska, patients receive compassionate, high-quality restorative care designed to bring back strength, comfort and confidence to their smiles.
Restorative dentistry focuses on repairing, rebuilding and replacing dental structures that have become compromised. Whether you’re dealing with a minor cavity or multiple missing teeth, Onalaska Smiles Dental offers personalized treatment plans using advanced techniques and materials to restore your oral health for the long term.
What Is Restorative Dentistry?
Restorative dentistry is a branch of dental care that addresses problems like decay, damage or tooth loss and restores your mouth’s function and appearance. These treatments help you chew more comfortably, speak clearly and prevent future dental problems. Instead of simply covering up issues, restorative dentistry fixes the underlying causes that can affect long-term oral health.
At Onalaska Smiles Dental, restorative care is customized to meet the needs of each patient, with a focus on comfort, durability and aesthetics. Whether you need one small repair or a more comprehensive restoration, the team is equipped to help you achieve a healthy smile that feels good and looks natural.

Common Restorative Dental Services Offered
Onalaska Smiles Dental provides a wide range of restorative treatments to help address different dental challenges:
Tooth-Colored Dental Fillings
When a tooth has decay or minor damage, tooth-colored fillings restore structure and function while blending seamlessly with your natural teeth. These fillings help stop decay from progressing and strengthen weakened areas.
Dental Crowns
Crowns are custom caps that cover and protect teeth that are cracked, worn or weakened. They restore the tooth’s shape, strength and chewing ability, while also improving its appearance.
Dental Bridges
Bridges replace one or more missing teeth by anchoring artificial teeth to neighboring natural teeth or dental implants. This helps maintain proper bite alignment, prevent surrounding teeth from shifting and improve chewing function.
Dentures & Partials
For patients missing multiple teeth, dentures or partial dentures provide removable solutions. These custom-made prosthetics help restore chewing ability, speech and the natural shape of your smile for enhanced comfort and confidence.
Dental Implants
Dental implants are a long-lasting solution for missing teeth. They act like natural tooth roots and support crowns, bridges or implant-supported dentures. Implants help preserve jawbone health while restoring normal function.
Root Canal Therapy
Root canal therapy saves teeth that are infected or painful by removing infected tissue and sealing the tooth to prevent further damage. This treatment resolves pain and keeps your natural tooth in place when possible.
Full Mouth Reconstruction
In more extensive cases — such as widespread damage, multiple missing teeth, or functional bite issues — full mouth reconstruction combines several restorative treatments into one comprehensive plan. This approach restores both form and function for long-lasting results.
Why Restorative Dentistry Matters
Restorative dentistry is more than fixing teeth — it supports overall oral health and quality of life. Here’s how restorative treatments can make a big difference:
Restores Function and Comfort
Missing or damaged teeth can make chewing and eating painful or difficult. Restorative treatments strengthen your bite and restore normal mouth function, so you can enjoy foods without discomfort.
Prevents Future Dental Problems
Addressing decay and missing teeth early helps protect the surrounding teeth and gums from shifting, gum disease, infection and further damage.
Boosts Confidence
A healthy, complete smile can improve your self-esteem. Many patients feel more comfortable smiling, speaking, and interacting socially after restorative treatment.
Supports Facial Structure
Teeth help maintain the structure of your face. Replacing missing teeth helps prevent bone loss and a sunken appearance over time, preserving your natural facial contours.
Enhances Speech
Missing or severely damaged teeth can affect the way you speak. Restorative care helps improve clarity and confidence when talking, connecting with others or presenting in public.
What to Expect at Your Visit
A visit to Onalaska Smiles Dental for restorative care begins with a comprehensive dental evaluation. The team reviews your dental history, examines your mouth and may take X-rays to understand the full scope of your needs.
From there, you’ll receive a personalized treatment plan that explains:
- Recommended restorative procedures
- How each treatment supports your oral health
- The expected timeline for care
- Post-treatment guidance and maintenance
The dental team uses advanced techniques and high-quality materials to ensure results that are durable, functional, and natural in appearance. Patient comfort and confidence are priorities throughout every step of the restorative process.
Serving the Onalaska Community
Onalaska Smiles Dental proudly serves patients in Onalaska and nearby communities. With a welcoming environment and a commitment to personalized care, the practice supports patients of all ages — from younger adults with decay or damage to seniors seeking tooth replacement options.
Whether you need a simple filling or a comprehensive smile restoration, Onalaska Smiles Dental offers reliable solutions designed to help you improve your oral health and restore your confidence.
Ready to Restore Your Smile?
If dental issues are affecting your comfort, function or confidence, restorative dentistry at Onalaska Smiles Dental can help you rebuild a healthy, strong smile.
Contact us today to schedule your appointment.
- Comprehensive Dental Care in Onalaska
December 15, 2025Dental Care in Onalaska; A healthy smile is an important part of overall wellness, confidence and daily comfort. For individuals and families seeking dependable dental care in Onalaska, Onalaska Smiles Dental provides comprehensive services designed to support long-term oral health. With a focus on preventive care, modern dentistry and patient comfort, the practice serves the Onalaska community with personalized, high-quality dental care for patients of all ages.
Family & General Dentistry in Onalaska
Onalaska Smiles Dental offers complete family and general dentistry, making it easy for patients of all ages to receive consistent care in one convenient location. Regular dental visits help prevent oral health issues and ensure healthy teeth and gums throughout every stage of life.
General dentistry services include:
- Routine dental exams
- Professional teeth cleanings
- Fluoride treatments
- Preventive care planning
- Tooth extractions when necessary
Families in Onalaska value having a trusted dental home where children, teens, adults, and seniors can all receive gentle, thorough care in a welcoming environment.
Preventive Dentistry for Lifelong Oral Health
Preventive care is the foundation of a healthy smile. Onalaska Smiles Dental emphasizes preventive dentistry to help patients avoid dental problems before they become more serious or costly.
Preventive services include:
- Comprehensive dental exams and cleanings
- Gum and periodontal evaluations
- Oral hygiene education
- Fluoride treatments to strengthen enamel
By prioritizing preventive care, patients in Onalaska can reduce the risk of cavities and gum disease while maintaining strong, healthy smiles for years to come.

Cosmetic Dentistry to Enhance Your Smile
A confident smile can positively impact personal, social, and professional life. Onalaska Smiles Dental offers cosmetic dentistry services to help patients improve the appearance of their teeth and feel confident when they smile.
Cosmetic treatments include:
- Professional teeth whitening
- Porcelain veneers
- Cosmetic bonding
These services address concerns such as discoloration, chips, gaps, and uneven teeth. Each cosmetic treatment is customized to deliver natural-looking results that complement the patient’s facial features and smile goals.
Restorative Dentistry for Damaged or Weakened Teeth
When teeth are damaged due to decay, injury, or wear, restorative dentistry helps restore strength, function, and appearance. Onalaska Smiles Dental provides restorative solutions designed to improve comfort and protect long-term oral health.
Restorative services include:
- Tooth-colored fillings
- Dental crowns to strengthen compromised teeth
- Bridges for replacing missing teeth
- Dentures and partial dentures
- Root canal therapy
These treatments help patients in Onalaska chew comfortably, speak clearly, and maintain a confident smile.
Dental Implants for Tooth Replacement
Missing teeth can affect oral function, facial structure and confidence. Onalaska Smiles Dental offers dental implants as a durable and natural-looking tooth replacement option.
Dental implants help patients:
- Restore chewing and bite function
- Maintain jawbone health
- Improve smile appearance
- Enjoy long-lasting comfort and stability
Dental implants provide Onalaska patients with a reliable solution that looks and functions like natural teeth.
Orthodontics & Smile Alignment in Onalaska
Properly aligned teeth contribute to better oral hygiene, improved bite function, and enhanced confidence. Onalaska Smiles Dental offers orthodontic and smile alignment solutions, including clear aligners, to help patients achieve straighter smiles.
Orthodontic care helps:
- Make teeth easier to clean
- Reduce the risk of tooth decay and gum disease
- Correct bite issues
- Improve smile aesthetics
Clear aligners provide a discreet and effective option for teens and adults seeking a more confident smile without traditional braces.

Patient-Focused Dental Care in Onalaska
Onalaska Smiles Dental is committed to providing a comfortable and supportive patient experience. The dental team takes time to listen, explain treatment options and create personalized care plans based on individual needs. This patient-centered approach helps reduce anxiety and ensures patients feel informed and confident about their dental care.
Why Onalaska Residents Choose Onalaska Smiles Dental
Patients in Onalaska trust Onalaska Smiles Dental because of its:
- Comprehensive dental services for all ages
- Strong focus on preventive care
- Cosmetic and restorative treatment options
- Orthodontic and tooth replacement solutions
- Comfortable, patient-centered environment
- Commitment to long-term oral health
Whether visiting for a routine check-up or advanced dental care, patients can expect consistent, high-quality treatment.
Your Smile Deserves Quality Dental Care in Onalaska
Oral health is essential for overall wellness and confidence. With comprehensive dental services at Onalaska Smiles Dental, patients in Onalaska can enjoy preventive, cosmetic, restorative and orthodontic care designed to support healthy, beautiful smiles for years to come.
Contact us today to schedule your appointment.
- Comprehensive Family Dentistry in Onalaska
November 19, 2025Family Dentistry in Onalaska; Finding a trusted family dentist in Onalaska is essential for maintaining lifelong oral health. Onalaska Smiles Dental stands out as one of the most reliable and comprehensive dental clinics in Onalaska. With a strong focus on patient comfort, modern technology and full-service dental care, this practice has become a favorite among families looking for gentle, affordable and high-quality dentistry.
Whether you need preventive care, restorative treatment, cosmetic enhancements or emergency dental services, Onalaska Smiles Dental is committed to helping you achieve a healthy confident smile.
Comprehensive Preventive Dentistry in Onalaska
Strong oral health starts with prevention and Onalaska Smiles Dental provides a wide range of preventive dentistry services to keep your smile healthy year-round. Their preventive care includes:
- Routine cleanings and dental exams.
- Oral cancer screenings.
- Digital X-rays for accurate diagnosis.
- Fluoride treatments to strengthen enamel.
- Dental sealants for cavity protection.
- Periodontal (gum) evaluations.
These services help detect issues early and prevent future dental problems. Families in Onalaska can rely on regular checkups at Onalaska Smiles Dental to maintain long-term oral health.
Cosmetic Dentistry in Onalaska for a Brighter, More Confident Smile
If you’re looking to enhance your smile, Onalaska Smiles Dental offers several cosmetic dentistry treatments designed to improve aesthetics while maintaining a natural look:
- Professional teeth whitening.
- Porcelain veneers to fix chips, gaps and discoloration.
- Cosmetic bonding for small cracks, uneven edges and minor tooth repairs.
- Smile makeover treatments customized to your goals.
Residents searching for a cosmetic dentist in Onalaska rely on this clinic for their expertise, artistry, and beautiful results.

Restorative Dentistry in Onalaska
Damaged or missing teeth can affect your confidence, comfort, and ability to chew properly. Onalaska Smiles Dental provides high-quality restorative dentistry solutions, including:
- Dental implants for long-lasting tooth replacement
- Crowns and bridges to restore function and appearance
- Tooth-colored fillings for natural-looking cavity repair
- Partial and full dentures
- Root canal therapy to save infected teeth
People in Onalaska trust this clinic for durable, comfortable and aesthetic restorative results.
Emergency Dental Care in Onalaska
Dental emergencies happen unexpectedly, and having a reliable emergency dentist in Onalaska is essential. Onalaska Smiles Dental provides urgent care for:
- Severe tooth pain
- Broken or cracked teeth
- Knocked-out teeth
- Lost fillings or crowns
- Infections and swelling
Helping patients get relief quickly and safely.
Children’s Dentistry in Onalaska
Families appreciate that Onalaska Smiles Dental warmly welcomes children. Their pediatric dentistry services include:
- Gentle cleanings and exams
- Fluoride treatments
- Dental sealants
- Education on brushing and flossing
- Cavity prevention care
Parents looking for a kid-friendly dentist in Onalaska trust this office for its welcoming environment and patient, compassionate team.
Why Onalaska Residents Choose Onalaska Smiles Dental
Here are some of the main reasons families choose this clinic as their primary dental home:
- Local convenience: serving the Onalaska community
- Full-service dental care: all treatments—from preventive to cosmetic to restorative—under one roof
- Experienced, friendly team: patients feel welcomed, heard, and cared for
- Affordable payment options: most major insurance plans accepted with flexible financing available
- Relaxed, comfortable environment: perfect for kids, adults, and patients with dental anxiety

Oral Health Tips for Onalaska Families
To maintain a healthy smile between visits:
- Brush twice daily using a fluoride toothpaste
- Floss every day
- Limit sugary snacks and drinks
- Stay hydrated
- Schedule regular dental checkups
- Ask about mouth-guards if you grind your teeth or play sports
Consistent care at home and at the dental office helps keep your smile strong year-round.
Your Trusted Family Dentist in Onalaska
If you’re searching for a dependable, caring, and experienced dentist in Onalaska, Onalaska Smiles Dental is a top choice. Their commitment to high-quality dentistry, modern technology, and exceptional patient comfort makes them a trusted name in the community.
From preventive care and cosmetic treatments to restorative solutions and emergency services, they are dedicated to helping every patient achieve their best smile.
Contact us today to schedule your appointment.
- Toothache Troubles And What To Do
October 9, 2023We’ve all been there – that sharp, throbbing pain in your tooth that seems to come out of nowhere. Toothaches can be excruciating, and they always seem to strike at the most inconvenient times. But fear not, because in this blog post, we’re going to explore the common causes of toothaches and provide you with some essential tips on what to do when you find yourself in the midst of toothache troubles.
Common Causes of Toothaches
Toothaches can be caused by various factors, but some of the most common culprits include:
- Tooth Decay: Cavities or dental caries are a leading cause of toothaches. When the enamel on your tooth is damaged, it exposes the sensitive inner layers, leading to pain and discomfort.
- Gum Disease:Infections and inflammation of the gums can cause discomfort and, in advanced stages, even toothaches.
- Tooth Sensitivity: Some people experience toothaches when consuming hot or cold foods or beverages due to tooth sensitivity. This can be caused by gum recession or enamel erosion.
- Dental Abscess: A dental abscess is a pocket of pus that forms due to a bacterial infection. It can be incredibly painful and requires immediate attention.
- Bruxism (Teeth Grinding): Grinding your teeth, especially at night, can lead to toothaches and jaw pain.
- Cracked or Fractured teeth: A cracked or fractured tooth can cause intermittent or constant pain, depending on the severity of the damage.
- Impacted Wisdom Teeth: Wisdom teeth that don’t have enough room to emerge properly can cause intense pain and pressure.
What To Do When You Have a Toothache
- Rinse Your Mouth:Start by gently rinsing your mouth with warm water to remove any debris that might be causing irritation. Be careful not to use hot or cold water, as extreme temperatures can exacerbate the pain.
- Floss: Carefully floss around the affected tooth to remove any food particles or plaque that may be contributing to the pain. Sometimes, a toothache can be as simple as something stuck between your teeth.
- Over-the-Counter Pain Relief: Over-the-counter pain relievers like ibuprofen or acetaminophen can help manage the pain while you seek professional dental care. Follow the recommended dosage on the label.
- Topical Anesthetics: Some pharmacies sell over-the-counter topical gels or ointments specifically designed for oral pain relief. These can provide temporary relief.
- Avoid Certain Foods: Stay away from extremely hot, cold, or sweet foods that can exacerbate the pain. Stick to soft, easy-to-chew foods.
- Apply a Cold Compress: Placing a cold compress on the outside of your cheek for 15-20 minutes can help reduce swelling and numb the area, providing some relief.
When to See a Dentist
While these home remedies can help manage the pain temporarily, they are not a substitute for professional dental care. It’s crucial to schedule an appointment with your dentist if:
– The pain persists for more than a day or two.
– The pain is severe and accompanied by other symptoms like fever or swelling.
– You have a history of heart issues or clotting disorders, as tooth infections can sometimes lead to more severe systemic issues.
Remember, toothaches are a sign that something is not right with your oral health. Ignoring the pain can lead to more significant problems down the road. Early intervention by a dentist is the key to preventing complications and getting you back to a pain-free, healthy smile.
In conclusion, toothaches can be incredibly distressing, but knowing what to do when they strike can help alleviate the pain and get you on the path to recovery. Don’t hesitate to reach out to your dentist for professional care and guidance, as they can provide the most effective solutions for your specific situation.
- Resisting Cavities: Your Guide to a Healthy Smile
September 9, 2023Understanding Cavities
Cavities, also known as dental caries or tooth decay, are small holes that form in your teeth when they become damaged or demineralized. They are typically caused by plaque, a sticky film of bacteria, which produces acid that eats away at the enamel – the protective outer layer of your teeth. If left untreated, cavities can grow larger and cause various dental problems, including pain, infection, and tooth loss.
Resisting Cavities
The good news is that you can take several steps to resisA beautiful smile can light up a room and boost your confidence. However, maintaining healthy teeth and gums is not just about aesthetics; it’s crucial for overall well-being. One common dental issue that can threaten your smile is cavities. In this blog post, we’ll explore what cavities are, their causes, and, most importantly, how to resist them and keep your smile shining.
maintain a healthy smile. Here are some effective strategies:
- Maintain Good Oral Hygiene:
The foundation of cavity prevention is practicing good oral hygiene. This includes:
– Brushing your teeth at least twice a day with fluoride toothpaste.
– Flossing daily to remove food particles and plaque from between your teeth.
– Using an antimicrobial mouthwash to kill bacteria and freshen your breath.
- Choose the Right Toothbrush and Toothpaste:
Selecting the right toothbrush and toothpaste can make a significant difference. Opt for a soft-bristle toothbrush to avoid damaging your enamel, and choose a toothpaste that contains fluoride, which helps strengthen your teeth.
- Balanced Diet:
Your diet plays a crucial role in cavity resistance. Limit your consumption of sugary and acidic foods and drinks. Opt for a well-balanced diet rich in fruits, vegetables, and dairy products, which provide essential nutrients for strong teeth.
- Stay Hydrated:
Drinking water helps maintain the proper pH balance in your mouth, which can reduce the risk of cavities. It also washes away food particles and bacteria.
- Regular Dental Checkups:
Don’t underestimate the importance of regular dental checkups. Your dentist can identify cavities in their early stages and provide preventive treatments like dental sealants and fluoride treatments.
- Dental Sealants:
Dental sealants are protective coatings applied to the chewing surfaces of your molars and premolars. They create a barrier against bacteria and acids, reducing the risk of cavities in these vulnerable areas.
- Fluoride Treatments:
Fluoride treatments can strengthen your tooth enamel, making it more resistant to acid attacks. Your dentist may recommend professional fluoride treatments, especially if you’re at higher risk for cavities.
- Avoid smoking and excessive Alcohol:
Smoking and excessive alcohol consumption can lead to dry mouth, which increases the risk of cavities. Quitting these habits can help protect your oral health.
Conclusion
Resisting cavities is essential for maintaining a healthy, beautiful smile. By following these strategies and making good oral hygiene a part of your daily routine, you can significantly reduce the risk of developing cavities. Remember, prevention is the key to a lifetime of good oral health. So, start taking care of your teeth today, and your smile will thank you for years to come.
- Defeating Tooth Decay
August 9, 2023A beautiful, healthy smile can light up your world. However, maintaining those pearly whites can be challenging, thanks to the ever-looming threat of tooth decay. Tooth decay, also known as dental caries or cavities, is a common dental problem that affects people of all ages. In this blog post, we’ll dive into the world of tooth decay, its causes, and how you can keep your smile content and cavity-free.
Understanding Tooth Decay
Tooth decay is a dental condition in which bacteria, acids, and poor oral hygiene erode the hard tissues of your teeth. It typically begins with the demineralization of the tooth enamel – the outermost layer of your teeth—and can progress to affect the inner layers of the tooth, leading to pain, infection, and, in severe cases, tooth loss.
The Causes of Tooth Decay
Tooth decay is primarily caused by the interaction of bacteria, sugars, and acids in your mouth. Here’s how it happens:
- Bacteria: Your mouth naturally contains bacteria, some of which feed on the sugars in the food you eat. As they consume these sugars, they produce acid as a byproduct.
- Acid Production: The acids produced by these bacteria attack the tooth enamel, weakening it and creating microscopic holes in the surface.
- Plaque Formation: The weakened enamel is more prone to bacterial adhesion, which leads to the formation of plaque, a sticky film on your teeth.
- Acid Attack: Plaque continues to produce acid, causing further damage to the enamel and ultimately creating cavities.
Preventing Tooth Decay
The good news is that you can take several measures to prevent tooth decay and enjoy a content, healthy smile.
- Brush and Floss Regularly:
The foundation of good oral health is consistent brushing and flossing. Brush your teeth at least twice a day with fluoride toothpaste and floss daily to remove food particles and plaque.
- Opt for the Right Dental Products:
Choose a soft-bristle toothbrush to avoid enamel damage and use toothpaste with fluoride, which helps strengthen your teeth.
- Maintain a balanced Diet:
Limit sugary and acidic foods and beverages in your diet. Instead, consume a well-balanced diet rich in fruits, vegetables, and dairy products to provide essential nutrients for strong teeth.
- Stay Hydrated:
Drinking water helps maintain a healthy pH balance in your mouth and washes away food particles and bacteria.
- Regular Dental Checkups:
Don’t underestimate the importance of regular dental checkups. Your dentist can catch cavities in their early stages and provide preventive treatments such as dental sealants and fluoride applications.
- Dental Sealants:
Dental sealants provide a protective barrier on the chewing surfaces of molars and premolars, reducing the risk of cavities in these susceptible areas.
- Fluoride Treatments:
Professional fluoride treatments can strengthen your enamel and make it more resistant to acid attacks, particularly if you’re at higher risk for cavities.
Conclusion
Tooth decay is a common dental issue, but with proper care and preventive measures, you can maintain a content, cavity-free smile. Your oral health plays a significant role in your overall well-being, so don’t neglect it. By following the tips and strategies outlined in this blog post, you can enjoy the confidence and joy that come with a healthy, content smile. Remember, prevention is the key to a lifetime of good oral health and happy, content smiles.
- Invisalign® Clear Aligners Offer Discreet Orthodontic Treatment
July 9, 2023A beautiful smile is a powerful asset, but many individuals hesitate to pursue orthodontic treatment due to concerns about the appearance of traditional braces. Fortunately, modern advancements in orthodontics have provided a solution that not only straightens teeth effectively but does so discreetly. In this blog post, we will explore the wonders of Invisalign® clear aligners and how they offer a discreet orthodontic treatment option.
The Challenge of Traditional Braces
Traditional metal braces have been a trusted method for straightening teeth for decades, but they come with some drawbacks. For many, the most significant concern is their highly visible appearance. Metal wires and brackets can detract from the natural beauty of your smile and make some individuals feel self-conscious during the treatment process. This is where Invisalign® clear aligners step in to revolutionize orthodontic care.
The Invisalign® Difference
Invisalign® is a revolutionary orthodontic treatment option that offers a discreet, convenient, and comfortable way to achieve a straight and healthy smile. Here are some key features and benefits of Invisalign®:
- Invisibility: Invisalign® clear aligners are virtually invisible. They are made of clear, medical-grade plastic and custom-fitted to your teeth, making them almost undetectable when you smile or speak.
- Removable: Unlike traditional braces, Invisalign® aligners are removable. This means you can take them out when you eat, brush, and floss, allowing you to maintain better oral hygiene and enjoy your favorite foods without restrictions.
- Comfort: Invisalign® aligners are smooth and comfortable to wear. There are no wires or brackets to cause irritation or discomfort, making them an excellent choice for individuals with active lifestyles.
- Effective Treatment: Invisalign® can effectively treat a wide range of orthodontic issues, including crowding, spacing, overbites, underbites, and more. Your orthodontist will create a personalized treatment plan to address your specific needs.
The Invisalign® Treatment ProcessThe journey to a straighter smile with Invisalign® involves several steps:
- Consultation: Your first step is to consult with an Invisalign®-trained orthodontist or dentist who will evaluate your smile and discuss your treatment goals.
- Custom Treatment Plan: Your provider will create a 3D digital image of your teeth and design a personalized treatment plan. You’ll get to see a virtual representation of your expected treatment outcomes.
- Clear Aligners: A series of clear aligners will be custom-made for you. You’ll wear each set for about two weeks, and they will gradually shift your teeth into their desired positions.
- Regular Checkups: You’ll have periodic checkups with your provider to monitor your progress and receive your new sets of aligners.
- Maintenance: Once your treatment is complete, your provider may recommend wearing a retainer to maintain your newly aligned smile.
Conclusion
Invisalign® clear aligners have transformed orthodontic treatment by offering a discreet and comfortable way to achieve a straighter smile. Say goodbye to the self-consciousness associated with traditional braces and hello to the confidence that comes with a beautiful, discreet solution. If you’ve been considering orthodontic treatment, consult with an Invisalign®-trained professional to see if this innovative treatment is the right choice for you. Your journey to a healthier, more beautiful smile starts here, and it’s as discreet as it gets!
- Dentures and Teeth Lost to Dental Trauma: A Second Chance for Your Smile
June 9, 2023A bright and confident smile can significantly impact our self-esteem and overall well-being. However, accidents, injuries, and dental trauma can sometimes lead to the loss of one or more teeth, leaving many individuals feeling self-conscious and in search of a solution. In this blog post, we will explore the world of dentures as a way to restore not only your smile but also your confidence and oral health after the loss of teeth due to dental trauma.
Understanding Dental Trauma
Dental trauma is a broad term that encompasses a range of accidents and injuries that can result in the loss of one or more teeth. Common causes of dental trauma include sports injuries, falls, vehicle accidents, and even biting into something hard. When teeth are lost due to dental trauma, it can lead to functional issues, such as difficulty chewing and speaking, as well as aesthetic concerns, impacting one’s self-esteem and quality of life.
The Role of Dentures
Dentures are a popular and effective solution for replacing missing teeth, especially when several or all teeth in an arch are lost due to dental trauma. Here’s a closer look at the different types of dentures and their benefits:
- Complete Dentures: Complete dentures are used when all teeth in one or both arches are missing. They consist of a full set of artificial teeth that are custom-made to fit the patient’s mouth perfectly. Complete dentures not only restore the appearance of a smile but also improve chewing and speaking abilities.
- Partial Dentures: When only some teeth are lost due to dental trauma, partial dentures are the solution. They are designed to fill in the gaps left by missing teeth by attaching to adjacent natural teeth or using dental implants for added stability.
- Implant-Supported Dentures: For a more secure and stable solution, implant-supported dentures are an excellent option. Dental implants are surgically placed into the jawbone, providing a strong foundation for dentures to attach to. This option offers superior stability and chewing efficiency.
The Benefits of Dentures
- Aesthetic Restoration: Dentures not only replace missing teeth but also restore your smile’s natural appearance, boosting your self-confidence.
- Functional Improvement: With dentures, you can once again enjoy your favorite foods, speak clearly, and maintain a balanced diet.
- Oral Health Maintenance: Dentures help prevent the shifting of adjacent teeth and the deterioration of jawbone, which can occur when teeth are missing.
- Custom Fit: Modern dentures are custom-made to provide a comfortable and secure fit, ensuring that they stay in place during daily activities.
- Cost-Effective: Dentures are a cost-effective solution for restoring your smile after dental trauma compared to other treatments like dental implants.
Conclusion
Dental trauma can be a traumatic experience, but dentures offer a second chance at a beautiful and functional smile. Whether you need complete dentures, partial dentures, or implant-supported dentures, modern dentistry provides solutions that can help you regain your confidence and oral health. With the proper care and maintenance, dentures can serve you well for many years, offering you the opportunity to smile, eat, and speak with confidence once again.
- Peak Oral Health: Healthy and Unhealthy Foods to Consume
May 9, 2023A confident smile is indicative of excellent oral health, and diet plays a significant role in attaining and maintaining that gleaming grin. Your diet can either promote healthy teeth and gums or exacerbate dental problems. In this article, we will discuss the effects of healthy and unhealthy diets on oral health, with the goal of achieving optimal oral health.
Nutritional Foods for Your Teeth
- Crunchy Fruits and Vegetables: Apples, carrots, and celery are not only nutritious but also aid in dental cleansing by stimulating saliva production and functioning as natural toothbrushes. They are able to remove food particles and plaque.
- Milk, cheese, and yogurt are excellent sources of calcium and phosphates, which aid in remineralizing teeth and strengthening tooth enamel. Additionally, they promote a balanced population of beneficial microorganisms in the pharynx.
- Lean Proteins: Foods such as poultry, lean beef, and fish are abundant in phosphorus, an essential mineral that, along with calcium, helps protect and strengthen your teeth.
- Nuts and Seeds: These provide essential nutrients such as calcium and phosphorus, and the act of gnawing on them stimulates saliva production, which aids in oral hygiene.
- Water: Maintaining hydration is essential for oral health. Water aids in the removal of food particulates, reduces the acidity in the mouth, and promotes the production of saliva, which contains vital minerals for the teeth.
Unwholesome Foods to Limit
- Sugary Snacks and Beverages: Sugary foods and beverages, such as candies, sodas, and fruit juices, promote the development of harmful microorganisms in the mouth, thereby causing tooth decay and cavities.
- Acidic Foods and Beverages: Foods rich in acid, such as citrus fruits, tomatoes, and carbonated beverages, can erode tooth enamel, making teeth more susceptible to damage.
- Foods like caramel and gummy candies can adhere to your teeth, making it simpler for bacteria to thrive on the sugars and generate acids that damage your teeth.
- Alcohol can cause parched mouth, which reduces saliva production and increases the risk of tooth decay and periodontal disease.
- Processed Foods: Oftentimes, highly processed foods contain added sugars and lack the nutritional value needed to support oral health.
Oral Hygiene practices
In addition to making wise food selections, there are practices that can aid in maintaining optimal oral health:
- Regular Brushing and Flossing: To remove plaque and food particulates, brush your teeth at least twice per day and floss daily.
- Regular Dental Checkups: Schedule routine dental examinations and cleanings in order to detect and treat any dental issues early.
- Limit grazing: Frequent grazing can increase your teeth’s exposure to acidic foods. Try to limit between-meal grazing.
- Fluoride strengthens tooth enamel and prevents dental caries.
- Don’t Forget Your Tongue: Brush or rasp your tongue gently to remove bacteria and maintain fresh breath.
The conclusion
In addition to sustaining an attractive smile, achieving optimal oral health involves preserving the health of your teeth and gums. Your dietary choices are crucial to the success of this endeavor. You can ensure that your smile remains healthy and confident for years to come by consuming tooth-friendly foods and minimizing your intake of toxic options, in addition to practicing good oral hygiene. Remember that a healthy smile reflects your own health!
